Hey guys! Long time follower first time poster. Since I was 13 or 14 my nipples have always been pointy (I can see them through any shirt) but to other people it's not incredibly noticeable. I have been lifting for 6 years, I have reduced my body fat and improved posture and it's helped alot. At 18 I was 140 18ish% bf now I'm 180 14ish% bf. Either way, I saw an endo around 8 months ago, he confirmed it was mild gyno, but he wasn't willing to experiment with any SERMS. And if there are studies showing SERMS don't have effect with gyno from puberty, I understand his reasoning (although I've never found one of those studies.) The reason I'm posting is because during my searching I found this article.
http://www.worldclassbodybuilding.com/forums/showthread.php?t=81608
I don't know who Eric potratz is, but he claims all gyno is reversible and that he did it with a ton of clients. What are your guys' opinions? Hopefully a Doc can chime in.
I notice that if I get above 15% bf my moobs become noticeable to everyone. Because of this, I have spent a lot of that past 6 years spinning my wheels. I try to bulk but once I hit a certain point my moobs pop and I panic and cut back down. I am 6'1" and was super lanky/ skinny fat. I picked up test-e (500mg/week as recommended by your well know members for a first cycle) liquidex and nolvadex. Partially because that article says there is a chance of reversing my gyno (don't worry I am super skeptical) but mostly because I want some size and I can't handle gaining fat too. I expect some people will tell me not to cycle and to bulk until I reach my genetic potential, but I hope I've explained why I don't want to do that so much.
My main questions are:
Do you think Eric Potratz's methods and reasoning for them are bs?
Is there anything soecial I should be watching for during this cycle since I got gyno during puberty?
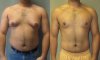
Here's some pictures. Do you guys think that since my gyno is mild, getting below 10% bf would be enough for them to not be noticeable?
(It might be hard to tell but the entire lower portion of my pet is fat, and like I said before I saw an endo and regardless of the fat, i don't have pseudogynecomastia)
Any replies would be extremely appreciated! Thanks guys!