The Transplanted Hairline
Hairlines created by modern hair transplant techniques use single hair follicles derived from the safe donor area (SDA). It is aptly noted that "a normal hairline is not a line at all, but rather a zone in which hairs become finer and more sparse as they gradually give way to the hairless forehead skin. This diminution in diameter and density is most prominent in younger patients, along temporal hairlines, and in female patients." In a transplanted hairline, which aims to mimic mild recession (Norwood class 2 or Norwood class 3), this observation becomes even more true. A receded hairline by nature assumes some miniaturization of the vanguard hair population.
The creation of a natural-looking hairline thus must include in the planning stages a deliberate attempt to add finer caliber hair in the very front of the hairline. Conventional hair transplantation, however, uses hair from the SDA that contains the thickest caliber hair in the entire scalp. In patients with especially thicker caliber hairs (eg, Asians) and in patients with darker hair color and a contrasting lighter skin color, the production of a natural, soft-looking hairline has remained a major challenge. The recognition of this problem has led to the grafting of bisected hair follicles into the hairline on the premise of thinner caliber hair growth. In the study using bisected hair follicles, wider application was limited by the poor yield (< 50%).
The advent of follicular unit extraction (FUE), which allows for in vivo extraction of single follicles without creating cosmetically significant scarring, has resulted in good results obtained in the frontal hairline. In addition, the technique increases the prospect of using single nonhead hair donor sources in transplantation. The FUE technique harvests hair follicle grafts through the use of punch devices to incise a circular path around individual follicular units from the epidermis into the dermis. However, the wider variation in the caliber of hair in the different body areas (finer leg hair to coarser beard hair) has created the possibility of a new approach to softer hairlines in the field of hair transplantation, particularly when head donor hair is not an option. For example, leg hair in most individuals possesses a finer caliber compared with most scalp hair populations.
These case reports demonstrate the successful transplantation of leg hairs to the hairline in 2 men who had undergone prior FUSS-FUT surgical procedures but who were dissatisfied with the unaesthetic results. In both instances, the source of dissatisfaction was in part from the use of thick caliber hair from the SDA of the head, which imparted a harsh hairline appearance. The primary advantage of using leg hair to rework hairlines is that it is relatively finer and thus can be used to fill in the vanguard regions of the hairline to create a much softer and more natural look.
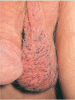
A, Prior to surgery to refine the hairline.
B, Four years after transplantation of leg hair, there is softening of the hairline.
Umar S. The Transplanted Hairline: Leg Room for Improvement. Arch Dermatol 2012;148(2):239-42. Arch Dermatol -- Abstract: The Transplanted Hairline: Leg Room for Improvement, February 2012, Umar 148 (2): 239
Background The large caliber of head hair in hair transplantation imparts a coarse hairline, whereas natural hairlines are typically softer. In hirsute individuals, transplantation of leg hair to the hairline may result in a superior aesthetic appearance.
Observation A total of 1025 leg hair follicles in 1 patient were grafted to an area 0.5 to 1.0 cm in front of and 0.5 to 1.0 cm internal to the vanguard hair of the original hairline and temporal recesses; the other patient received approximately 1000 leg hairs and 600 head hairs to advance and soften his hairline and to create a custom widow's peak. Transplantation resulted in a fully grown and soft-looking hairline after 9 months in the first patient, with growth of 75% to 80% of the transplanted leg hair. The mean length of the transplanted leg hair was longer than the length of the original leg hair, with less curliness but similar hair width. Transplanted leg hair width was significantly finer compared with existing head hair width. After 4 years, results were sustained, minimizing concerns that subsequent hair loss might result from leg hair cycle variations. In the second patient, similar results were observed at 3 years.
Conclusion The use of leg hair in transplantation provides additional options in patients with hairlines that need to be refined.